
Zoonotic diseases are infections that can spread between people and animals. They are caused by germs such as viruses, bacteria and parasites.
Individuals can get zoonotic diseases by direct contact with animals or by indirect contact with animal products. It can also be spread through bites from ticks or mosquitoes, and through contaminated food and water.
Zoonotic diseases: Rabies
Around a third of all the infectious diseases that affect humans are zoonotic. These range from gastrointestinal diseases mild, such as giardiasis, until the anger is deadly. Some zoonotic diseases are caused by viral infections, while others are caused by parasites or bacteria. All zoonotic diseases begin with animals and then they can be spread to humans through direct contact or exposure to infected animal or contaminated area.
Almost all human rabies cases in humans occur by the bite of an infected dog, but the raccoons, foxes, bats and other mammals also can cause the disease. The symptoms of rabies vary from person to person and can include early signs are nonspecific, such as fever, headache, and vomiting, followed by neurological signs of acute and, ultimately, death.
The people are at a higher risk of contracting zoonotic diseases when living or travelling in areas where wildlife abounds and livestock, such as forests or agricultural areas that are rural. Also at greater risk when visiting markets where they mix multiple animals from different parts of the world. These conditions allow the pathogen to circulate more freely.
The public health veterinarians are experts in the tracking and prevention of zoonotic diseases, but the risk reduction efforts should involve multi-disciplinary teams and a holistic concept of health for both human populations and for the animals. Prevention methods differ for each pathogen, but practices such as safe handling of food, clean water and sanitation, and vaccination can reduce the risk to the community.
Vaccines the rabies virus and some other zoonotic diseases are available for humans. Persons with immunosuppression (for a pre-existing condition or medications such as chemotherapy) have an especially high risk of contracting a zoonotic disease, and may experience a more severe disease and start quickly than people who do not have this comorbidity. Examples of immunosuppression include AIDS, which increases the likelihood of infection with the bacteria, Cryptosporidium parvum and causes severe disease and death.
It is believed that the global climate change, the excessive use of antimicrobials in human medicine and farming practices, more intensive contribute to the increase of the rate of zoonotic diseases. By continuing to collaborative practices, government agencies can strengthen their ability to respond to zoonotic diseases, new and emerging.

Zoonotic diseases: the monkeypox
Monkeypox is a rare and potentially mortal disease caused by infection with the virus of the pox. This virus is related to smallpox and can cause the same symptoms in humans: fever, fatigue, swollen lymph nodes and a rash that appears first on the face and then spreads throughout the body. The rash is formed by fluid-filled blisters that crust over, and then fall down. This rash can be easily confused with chickenpox or other disease outbreak.
Until recently, the majority of the cases of monkeypox were reported in central and west Africa, where the disease is endemic, but in 2022, the outbreak of monkeypox has been expanded all over the world, including areas where the disease usually does not occur.
The World Health Organization (WHO) has published guidelines and resources for health professionals about the outbreak. The organization also provides guidance to persons who have a high risk of contracting the virus. These include people who live or work in areas where the disease is present, people who are in close contact with someone who has monkeypox confirmed and pregnant women. The who recommends that any person who develop the signs and symptoms of smallpox seek medical attention immediately.
Although most people recover without treatment, the complications can be serious and potentially life threatening. These may include bleeding, the development of severe rashes that are blended or sepsis. Pregnant women, children and people with weakened immune systems are more likely to suffer severe illness or die.
The transmission of monkeypox is spread most commonly from person to person through contact with skin lesions or blood of an infected person, but it can also occur when a person coughs or sneezes and the droplets are transported by the air. The virus can also be transmitted through the transmission fecal.
People with greater risk of developing a severe case of monkeypox should isolate themselves at home until the skin lesions have healed completely. The WHO says that it is also important to avoid pregnancy and lactation if one has been in contact with an infected person. If a pregnant woman is in isolation develops symptoms of the disease, your doctor should consider the induction of labor or cesarean section only when it is based on obstetric indications and the preference of the patient.
Zoonotic diseases: Lyme disease
The growing use of domestic animals (including pets), as well as the increase of the handling, transport and trade (legal and illegal) of these animals, increasing the risk of zoonotic diseases. In addition, the shortening of the incubation periods means that pathogens can move around the world more quickly. In consequence, a greater percentage of new infectious diseases are zoonotic.
For example, in the united States, most of the Lyme disease is transmitted by ticks carrying the bacterium Borrelia burgdorferi in the northern regions of the united States (so-called “hot spots”). The tick is also responsible for transmitting B burgdorferi to dogs but not to humans. Other ticks can be vectors of Lyme disease, but infection rates lower.
Generally, the earliest symptom of Lyme disease is an injury to feature in the form of diana. The center of this rash usually disappears as the disease progresses; however, some patients may experience a clearance, central part later in the course of the disease.
In the united States, children under the age of 15 years and men aged from 40 to 60 years are more likely to develop Lyme disease, possibly because they spend more time outdoors. The emergence of Lyme disease has increased substantially since the beginning of the 1990s, and the majority of cases occur in the northeast and the mid-Atlantic region. This has been attributed to changes in the environment, including a reduction in the deer population, and the planting of more trees.
The treatment of zoonotic infections often involves the administration of antibiotics. Recommended antibiotics such as doxycycline or amoxicillin for initial therapy in adult non-pregnant women with Lyme disease early. Cefuroxime axetil and azithromycin are alternative choices for those allergic to penicillins.
You should take a detailed history, with special attention to the travel, vaccination status, and hobbies. Other important points of the anamnesis, which include a review of pets, other exposures to animals and diet. Often it takes a laboratory evaluation detailed, which include CBC with differential for lymphocytosis (in influenza and brucellosis), leukopenia (in COVID-19 and TB resistant to rifampicin), thrombocytopenia (in Coxiella and RMSF) and eosinophilia in trichinellosis.
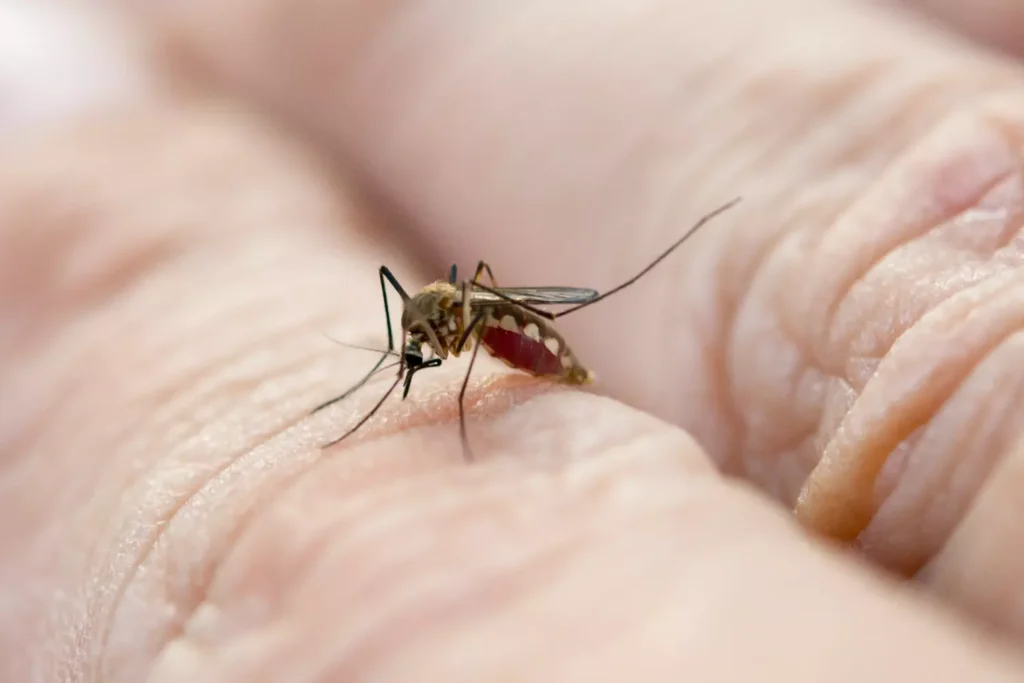
Zoonotic diseases: West Nile Virus (WNV)
The West Nile virus is one of the few zoonotic diseases transmitted by mosquitoes that can cause encephalitis (inflammation of the brain). Most people with west nile virus experience only mild symptoms such as fever, headache, and fatigue. However, if a person's immune system is compromised, the infection can be fatal. People over the age of 60 years and those with certain medical conditions such as cancer, hypertension, diabetes, kidney disease, or an organ transplant have a higher risk of becoming severely ill with WNV.
The most common cause of the VNO is the bite of an infected mosquito. The virus spread by mosquitoes that get it from infected birds, especially crows and jays. Then, mosquitoes transmit the virus to other birds and humans when they bite. In rare cases, the virus can also spread through a blood transfusion or an organ transplant, or from the mother to the fetus.
If someone you suspect that you have a WNV infection, a doctor will order a blood test to measure antibodies against the virus. In most cases, the presence of these antibodies is sufficient to confirm the diagnosis. However, if the symptoms are severe or involve the brain, doctors can perform a lumbar puncture to determine the severity of the infection and take steps to cure it. During this procedure, a needle is inserted into the column to remove cerebrospinal fluid, which can reveal the presence of the virus in the brain and the spinal cord. The magnetic resonance imaging and other imaging tests may also help to detect the inflammation of the brain.
The majority of people who contract west nile virus recover on their own, and the-counter pain medications, such as acetaminophen and ibuprofen, can relieve the discomfort of the symptoms. Patients who develop WNV neuroinvasivo require hospitalization and supportive care may include intravenous fluids, and respiratory support.
The best way to prevent the West Nile Virus (WNV) it is protected from mosquitoes. Wear long sleeves and pants when outdoors, and apply insect repellent with a minimum of 20 percent DEET (N,N-dietilmetatoluamida) in the exposed skin. Make sure that the doors and windows of your house have mosquito nets tight and if you are in a bad condition be sure to repair any hole they have. In addition to report any dead birds to your agency and local health do not touch them, as they can easily transmit the virus to mosquitoes.